Complete Spine and Pain Care is committed to providing excellence in comprehensive pain management services. In keeping with our mission, our staff is dedicated to working with you in a supportive and friendly environment to develop a treatment plan tailored to your particular diagnosis and needs.
We try to avoid surgery at all costs and have numerous non-surgical and alternative treatments for your Sciatica.
Under the leadership of Janet D. Pearl, M.D., M.Sc. we utilize an integrated, multidisciplinary team approach that facilitates superior pain care by drawing on the expertise of numerous highly trained professionals in a variety of specialties.
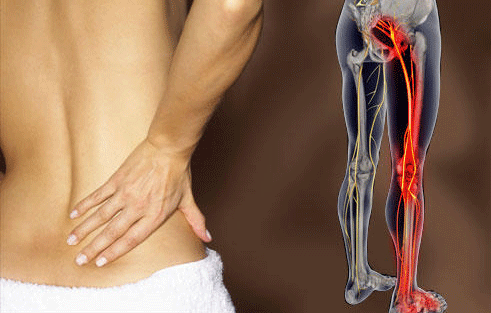
Sciatica is pain caused by irritation or compression of the sciatic nerve, usually felt in the lower back, buttock, and back of the leg.
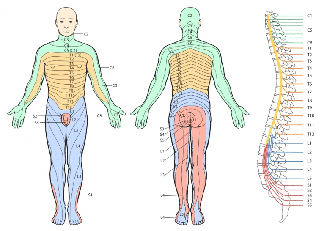
The sciatic nerve is the largest nerve in the body. There are two sciatic nerves, one on each side of the body. They begin in the lower back, where they are formed by the combination of five spinal nerves from the lower spine (the fourth and fifth lumbar spinal nerves and the first three sacral spinal nerves). They run from the lower back, through the buttock and down the thigh; they then divide into other nerves that provide sensation and muscle function in the lower legs and the feet. Sciatica can be felt anywhere along the course of the sciatic nerve.
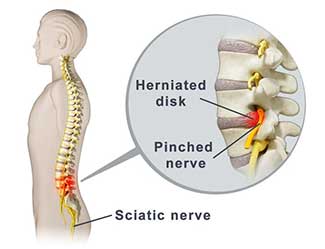
Sciatica is not a medical condition – it is a symptom of an underlying condition. Disturbances anywhere along the course of the sciatic nerve can give rise to sciatica. The most common cause is nerve compression at the spine, but injuries to the sciatic nerve in the lower pelvic cavity, buttock, and back of the thigh are also frequent.
Sciatica is usually caused by lower back problems, particularly by disorders of the spine, such as a herniated disc, intervertebral disc degeneration, displacement of vertebral bones, bone spurs, joint cysts, or narrowing of the spaces between vertebral bones. These disorders can cause the compression of the spinal nerves that form the sciatic nerve, leading to inflammation, pain and numbness in the affected leg.
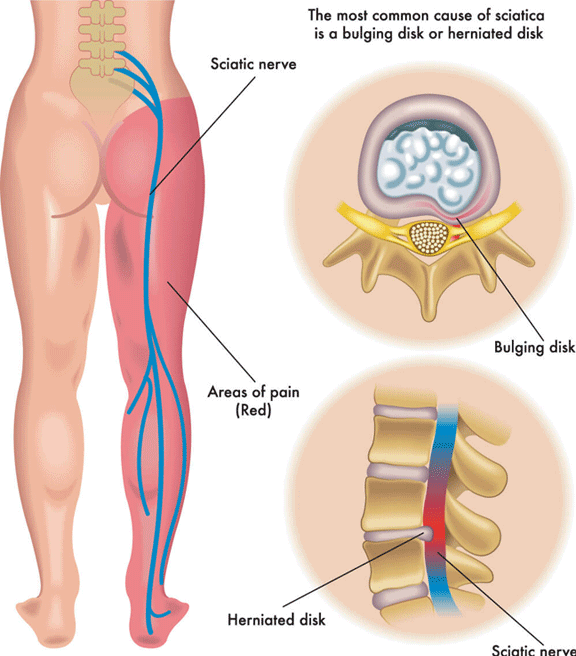
The vast majority of sciatica cases are due to intervertebral disc disorders. The intervertebral discs are structures located between the spinal bones (vertebrae). They have a soft center and a tough exterior, acting as cushions between the vertebrae, and allowing some mobility of the spine.
Over time, these discs dehydrate and become stiffer, losing their cushioning ability and leaving the nerves more susceptible to compression. When excessive pressure or stress is placed on the spine, the disc may be compressed to a point where it may tear or bulge outwards, creating a herniated disc. When this occurs in the lower back, it may cause inflammation or compression of a spinal nerve, leading to sciatica.
Occurrence rates vary significantly across studies, but the highest estimates indicate that sciatica may affect up to around 40% of individuals at some point in life. Since the vertebral discs tend to degenerate time, there is a higher risk of sciatica as one ages.
Obesity or excessive weight are risk factors for sciatica. Obesity increases the rate of spinal disc degeneration thereby leading to a higher incidence of disc lesions, as well as to earlier onset of age-associated disc conditions. The increased pressure on the lower spine due to excessive weight also increases the likelihood of disc injuries.
Work-related activities may also increase the probability of developing sciatica. Jobs that require harmful work postures, cause whole body vibration, or require physical loading or heavy lifting are among those more prone to the development of disc tears and herniations. Prolonged sitting on hard surfaces can also produce sciatica due to pressure on the sciatic nerve.
Smoking has also been associated with a higher risk of sciatica, most likely due to reduced blood flow to the lower spine, contributing to disc degeneration. Smoking associated coughing may also lead to injuries in the spinal discs.
Sciatica usually affects only one side of the lower body. Depending on where the sciatic nerve is affected, pain can be felt in the lower back, buttock, back of the thigh, and down the leg, sometimes reaching the lower leg and the foot. Typically, it is felt most intensely in the back of the thigh or in the buttock.
Sciatica may begin either suddenly with physical activity or slowly. It frequently goes away within a few weeks. However, depending on the cause, it may last longer, sometimes several months to years.
Sciatica pain intensity is variable. It is often continuous, severe and highly debilitating, but it can be intermittent and milder. Sciatica may also be felt as tingling, numbness, or weakness in the leg or legs. Intense pain due to sciatica is typically described as aching, sharp, searing, burning, shooting or as electrical shocks running down the leg. It usually worsens when standing or sitting, and decreases while walking or lying down.
When pain is severe, it may be difficult to stand up and walk. Sudden movements of the spine, such as sneezing or coughing may increase pain. Patients with sciatica may also experience muscle weakness in the affected leg. If progressive leg weakness occurs or difficulty with bowel or bladder function, then an urgent medical evaluation is necessary and your doctor may send you to a local emergency room should these symptoms.
For persistent sciatic pain, there are a number of drugs that can be used. Simple painkillers, including acetaminophen or non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be effective, depending on the cause of sciatica. When these methods are not effective, spinal corticosteroid injections may be needed.
In addition, for severe pain, opioids, such as codeine or oxycodone, tricyclic antidepressants, such as amitriptyline, or anticonvulsants, such as gabapentin or pregabalin, can be useful for treating pain and helping with sleeplessness caused by the pain.
Sciatica can be reduced by remaining physically active and doing simple exercises, such as walking and gentle stretching. Hot or cold compresses may also be helpful. Physical therapy or yoga may help improve posture, strengthen the muscles in the back, improve the flexibility of the spine, and thereby decrease pain.
Depending on the cause of sciatica, surgery may eventually be needed to correct spine problems that may be causing the compression of a nerve, for example.