Post-stroke pain
What is it?
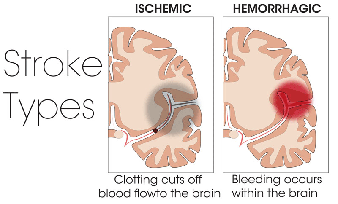
Post-stroke pain is pain that develops as a consequence of stroke. Stroke, also known as cerebrovascular accident, or more colloquially, brain attack, is characterized by the loss of blood flow to the brain. This may occur due to a blockage of a blood vessel (ischemic stroke) or due to bleed from a blood vessel (cerebral hemorrhage or hemorrhagic stroke). This loss of blood (and oxygen) supply causes injury in the brain that can have a number of consequences, one of which being the development of chronic pain. Post-stroke pain is therefore a type of neuropathic pain, i.e., pain arising from damage or dysfunction of the nervous system.
Post-stroke pain is a type of central pain, i.e., pain that originates primarily in the Central Nervous System. Injury to certain particular parts of the brain are a common direct cause of central post-stoke pain, but it can develop as a consequence of strokes occurring anywhere in sensory central nervous system structures. The most common areas of injury causing post-stroke pain are lesions in the thalamus (a brain structure that acts as a relay station for sensory and motor signals to the cerebral cortex) or in the somatosensory cortex (the region of the cerebral cortex that receives and processes sensory input from the body). There are many factors in the diagnosis of central post-stroke pain. Nevertheless, there are a number of criteria that aid in the diagnosis: onset of pain at or after stroke, pain within an area of the body corresponding to a brain injury and located on the stroke-affected side, and confirmation of a brain lesion. It is also diagnosed by exclusion, when other plausible causes of pain can be discarded.
Who gets it?
Central post-stroke pain occurs in patients who have suffered a stroke in areas of the central nervous system associated with sensory processing. Studies on the occurrence of central post-stroke pain indicate values ranging from 8% to 12% of stroke patients developing central pain.
The time until the onset of central post-stroke pain is highly variable, but it most commonly develops within 1 to 6 months of the stroke, with the highest occurrence being between 3 to 6 months after stroke. Nevertheless, it can even develop up to 10 years after stroke and it can persist for many years or even throughout life.
The prevalence rate of central post-stroke pain seems to have no relation with gender, age, or the location of the stroke.
What kind of pain results?
Post-stroke pain patients show common features of neuropathic pain: sensory abnormalities, increased reaction to painful stimuli (hyperalgesia), and pain in response to previously non-painful stimuli, such as touch (allodynia). Painful sensations may be diffuse or vary radically from one day to the next. Location, intensity, and duration of pain are other highly variable aspects of central post-stroke pain.
Pain is most commonly reported on the affected side of the body (the opposite side of the lesion). It is reported mainly in the extremities (hands and feet) in the form of pins and needles, tingling, burning pain, numbness, and less commonly as electric shocks, painful cold, and itching. Although it’s less common, pain may also develop more proximally, in the thighs or shoulders, for example. But pain may also affect the entire side of the body opposite to the lesion.
Post-stoke pain can be spontaneous, occurring with no discernable stimuli, or it can be evoked. Spontaneous pain is typically continuous, but it can also be intermittent, in this case being usually more severe, although the severity is also variable. Post-stroke pain increases with external stimuli such as stress, temperature changes, and movement, and can decrease with rest and distraction.
Central post-stroke pain must be differentiated from pain triggered by other mechanisms. It is common for other pain syndromes to also occur with post-stroke pain such as myofascial pain syndrome, complex regional pain syndrome, joint pain, or headache.
Terms often used by patients to describe central post-stroke pain include burning, aching, pricking, penetrating, lancinating, lacerating, shooting, freezing, squeezing, stabbing, and throbbing.

Treatment of post-stroke pain
Post-stroke pain management is often difficult to achieve. No standard treatments have been established and central post-stroke pain is usually resistant to conventional analgesic drugs. Treatment is often based on experimental trials, and pain relief is usually achieved by combining multiple drugs.
First-line approaches include tricyclic antidepressants (amitriptyline, nortriptyline, imipramine, or desipramine), selective serotonin and norepinephrine reuptake inhibitors (venlafaxine, duloxetine, desvenlafaxine, or milnacipran) and antiepileptic drugs (pregabalin, carbamazepine, lamotrigine, gabapentin, or levetiracetam). Opioids can also be used but there is little evidence of a beneficial effect and they are therefore usually not recommended due to their side-effects and addictive potential. Anesthetics (ketamine, lidocaine, or propofol) can also provide post-stroke pain relief, but their side-effects or the short-acting nature have limited their use. The tricyclic antidepressant amitriptyline is most often the drug of choice, since its efficacy in relieving central post-stroke pain has been consistently reported.
When post-stroke chronic pain is unresponsive to pharmacological treatment, brain stimulation approaches may be used. Motor cortex stimulation can modulate various cerebral structures and pathways involved in pain control and may provide satisfactory long-lasting pain relief in some patients. Deep brain stimulation, a surgical procedure that requires the insertion of electrodes in specific areas of the brain is also effective in many patients. Repetitive transcranial magnetic stimulation (rTMS), a non-invasive procedure that creates a brief high-intensity magnetic field, may also lead to a small but long-lasting pain relief in central post-stroke pain patients, thereby being useful in combination therapies.
Transcutaneous electrical nerve stimulation and acupuncture may also have beneficial effects, but their efficacy has not been extensively studied.
References
- Akyuz G, Kuru P (2016). Systematic Review of Central Post Stroke Pain: What Is Happening in the Central Nervous System? Am J Phys Med Rehabil [Epub ahead of print]. doi: 10.1097/PHM.0000000000000542
- Flaster M, Meresh E, Rao M, Biller J (2013). Central poststroke pain: current diagnosis and treatment. Top Stroke Rehabil, 20(2):116-23. doi: 10.1310/tsr2002-116
- Harrison RA, Field TS (2015). Post stroke pain: identification, assessment, and therapy. Cerebrovasc Dis, 39(3-4):190-201. doi: 10.1159/000375397
- Kim JS (2009). Post-stroke pain. Expert Rev Neurother, 9(5):711-21. doi: 10.1586/ern.09.19
- Klit H, Finnerup NB, Jensen TS (2009). Central post-stroke pain: clinical characteristics, pathophysiology, and management. Lancet Neurol, 8(9):857-68. doi: 10.1016/S1474-4422(09)70176-0
- Oh H, Seo W (2015). A Comprehensive Review of Central Post-Stroke Pain. Pain Manag Nurs, 16(5):804-18. doi: 10.1016/j.pmn.2015.03.002