Frozen Joint syndrome or Adhesive Capsulitis
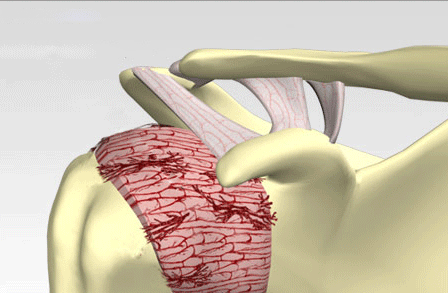
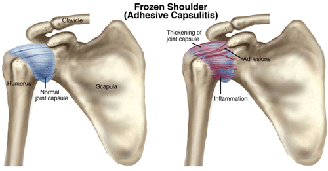
Frozen Joint syndrome or Adhesive Capsulitis is a painful disorder that causes decreased (ROM) range of motion in a joint (shoulder most often, knees or less often hips). This is thought to be caused from chronic inflammation, scarring, thickening and shrinkage of the capsule that surrounds the joint. Adhesive capsulitis is often seen following periods of immobilization of the affected joint, especially after extensive surgery. Adhesions are the fibrous bands of tissue that develop between joint surfaces. A decrease in the synovial fluid, may contribute to a loss of function. The shoulder joint is a ball and socket joint with the round head of the upper arm (humerus) fits into the socket of the scapula (shoulder blade). This socket area (capsule) can thicken and tighten leaving less room for movement and can cause stiffness.
Frozen shoulder causes are unknown (idiopathic). Frozen knee most often occur after a total knee replacement surgery or recent injury. Common risk factors can include: Age > 40 years, 70% are women, following a recent surgery or fracture with immobilization, Diabetics are 2-4x more likely to develop and may have more severe symptoms, CVA, Hyper/Hypothyroidism, elevated triglycerides, CAD, Parkinson’s disease, upper extremity paresis, brachial plexus injury or spinal cord injury can be contributory causes.
Symptoms: sharp pain early then becoming more of a dull ache over time. Pain or ache is felt in the affected joint especially with movement. Pain is often located over the outer shoulder and upper arm with frozen shoulder.
Phases of Frozen Joint Syndrome
There are typically 3 phases of Adhesive Capsulitis (frozen joint) syndrome:
-
- Pain—with a gradual onset of diffuse shoulder pain and stiffness that can last from weeks to months. Range of motion is usually preserved in this phase. The glenohumeral joint loses range of motion with external rotation, internal rotation and abduction (combing hair, reaching across body for objects or putting a car seat belt on.) Pain is often more severe at night and then progresses to continuous pain even at rest. Movement, psychological stress, exposure to cold or vibration and changes in the weather can worsen symptoms. This pain can last 2 months-9 years before entering phase two.
- Frozen– pain continues, but usually will decrease. Progressive stiffness and decreased ROM in all directions continues. Normal daily activities are affected. This phase can last 3-9 months or longer.
- Thawing– function and range of motion progressively improve over 12-24 months. Less than half of patients will continue with persistent range of motion limitations but only very few (10%) will have clinically significant long term functional limitations.
Treatment
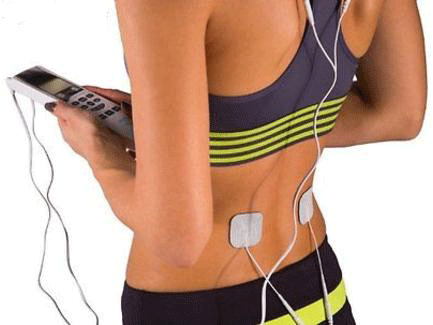
Frozen joint syndrome is usually curable (may take up to 3 years) and is focused on improving range of motion and strength in the joint. NSAIDs and topical analgesics can improve pain relief. Heat and cold therapy and TENS unit are helpful. Steroid joint injections or blocks can improve inflammation and pain at the joint and may be needed prior to starting Physical Therapy. Click here for home physical therapy exercises that you can do for your frozen shoulder. XRAY or MRI may be used confirm a diagnosis or rule out other causes.
Physical Therapy includes such exercises as passive stretching and external rotation, forward flexion of arms while lying down and stretching your arm across across the front of your body.
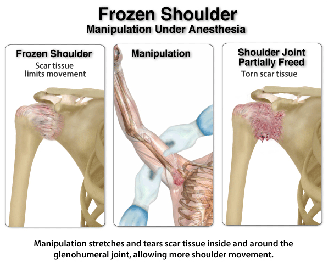
Surgery under general anesthesia – Manipulation or Arthroscopy may be recommended if less conservative treatments fail. The surgeon will forcefully break up the adhesions and move (manipulate) the joint. This procedure is followed up with Physical Therapy after surgery to continue to improve and maintain range of motion and prevent reformation of adhesions.